Type 1 diabetes can be such a scary diagnosis because not only is it often first discovered in children, but it can initially present with these kids becoming extremely sick without any obvious warning signs.
Type 1 diabetes affects about 1.25 million people in the United States. While American diabetes rates are outrageously high, type 1 is much less common than type 2 diabetes, representing only about 5% of all cases of diabetes mellitus (1,2).
Type 1 Diabetes Definition
Type 1 diabetes is an autoimmune disease that causes a deficiency in insulin.
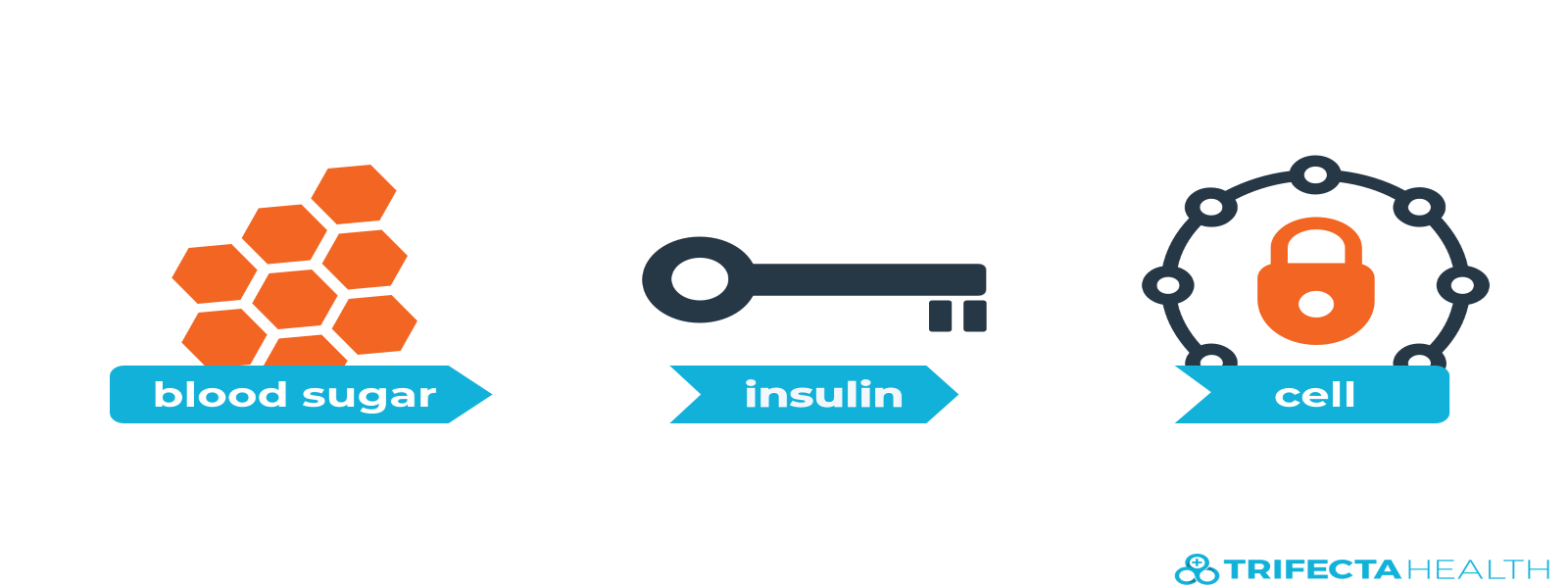
Glucose provides a basic energy source our body needs to function. It can be thought of as our fuel. In order for our bodies to use glucose, we need insulin. Insulin is a hormone made by an organ called the pancreas. Insulin can be thought of as the key needed for glucose to enter our cells.
Autoimmune diseases are conditions that involve the immune system attacking and damaging parts of it’s own body by mistake.
In type 1 diabetes, the immune system damages the pancreas.
More specifically the immune system attacks certain hormone producing islet cells in the pancreas, called beta cells, which are in charge of making insulin (3).
If some insulin is produced, it may not work correctly - a condition that is sometimes referred to as insulin resistance. However this is thought to be a more common problem in type 2 diabetics.
Juvenile Diabetes
Type 1 diabetes is classically thought of as a disease diagnosed in childhood and is one of the most common chronic diseases in children. It has therefore also been referred to as ‘juvenile diabetes’.
The recent unfortunate large surge in obese children has led to many developing type 2 diabetes. This can make the term ‘juvenile diabetes’ somewhat confusing as it may be almost as common for a child to have type 2 diabetes as type 1 diabetes.
Adult Onset Type 1 Diabetes
While type 1 diabetes is much more commonly diagnosed in children, any age can be struck by the disease. In fact, up to 25% of affected people develop the type 1 diabetes in adulthood (4, 5).
An adult with type 1 diabetes has similar symptoms as children, although they can sometimes develop less quickly. While each person can be different, there are people that continue making some insulin at first, early in their diagnosis. In rare cases, some early stage type 1 diabetics may not even require insulin right away. However they will eventually require insulin as part of their daily treatment regimen (6).
Type 1 Diabetes Symptoms
Type 1 diabetes can present in many ways.
Some less alarming initial symptoms may include:
- Tiredness
- Frequent Urination
- Excessive Thirst
- Weight Loss
- Blurry Vision
- General Weakness
- Frequent Infections
- Numbness and Tingling
Diabetes causes the immune system to not work as well, which means affected people often have an increased risk of infections. Because of this, something as simple as a yeast infection may be the first clue to the diagnosis (7).
Unfortunately, many of these less obvious symptoms are often not identified right away and type 1 diabetes can become severe very quickly.
Diabetic Ketoacidosis & Other Complications of Diabetes
In fact, many children aren’t diagnosed until they have developed a life-threatening complication called diabetic ketoacidosis (DKA) (8, 9).
With intensive treatment in the hospital, people with DKA usually get better. However it can recur in the future if the disease isn’t carefully managed on a daily basis.
Other serious complications that can be caused by diabetes include:
- Kidney Failure
- Heart Attacks
- Stroke
- Sexual Dysfunction
- Neuropathy
- Impaired Healing and Amputations
- Frequent and/or Chronic Infections
- Damaged Blood Vessels
Type 1 Diabetes Life Expectancy
Due to the complications discussed above, people with type 1 diabetes have been found to have a lower life expectancy and are at an overall higher risk of death compared to people without diabetes (10) .
A holistic health care approach to treatment that includes diet, exercise and aggressive insulin therapy can substantially reduce these risks allowing diabetics to live long and thriving lives.
Studies support this approach and show that people with consistently controlled sugars (represented by a lower HbA1c) have an overall lower risk for lifetime complications (11).
Type 1 Diabetes in Pregnancy
People who have type 1 diabetes and become pregnant are noted to have ‘pregestational diabetes’. This is different from ‘gestational diabetes’, which does not develop until after the woman becomes pregnant and usually goes away after she delivers her baby.
The overarching goal for type 1 diabetics is to keep the glucose levels to as near normal as possible - and this is also shown to minimize complications in pregnancy.
Diabetes is a risk factor for many pregnancy complications for both the mother and the baby including pre-eclampsia and congenital birth defects.
Therefore it is very important for diabetics to carefully follow their diet, exercise & medication regimens and perform more frequent blood tests with more frequent doctor visits for additional monitoring.
For additional information on diabetes in pregnancy, read this article.
Is Type 1 Diabetes Genetic?
It’s well-established that there is some hereditary component to developing diabetes. The risk of type 1 diabetes significantly increases if close relatives have the disease. For example, the risk of acquiring type 1 diabetes is 0.4% in people without any affected relatives but it may jump to as high as 10% if a sibling is affected and to as high as 30% if both parents have the disease (12 , 13 , 14) .
However, the genetic link appears to be very complicated and is likely influenced by many genes and other factors that are not yet fully understood (15).
A popular belief is that people who develop diabetes may have a genetic predisposition that is then activated by a trigger in the environment.
Type 1 Diabetes Causes
One of the most frustrating parts of type 1 diabetes is that there isn’t yet a good way to predict or prevent its development.
We know that type 1 diabetes is caused by damage to an organ called the pancreas, which produces insulin. This damage becomes so severe that the pancreas stops being able to produce insulin. It is almost always the result of an overactive immune system inappropriately attacking the pancreas.
What triggers the immune system to go awry? Like many things in medicine, this answer isn’t crystal clear to even the most skilled specialists.
Some suspected influences include: viral infections, neonatal influences, other environmental factors and genetics.Viral Infections
Some viral infections may trigger people who are genetically susceptible to develop the disease (16) .
Neonatal Influences
High birth weight and prematurity may also be risk factors (17).
Other Environmental Factors
Many other possible contributing environmental factors have been looked at including birth season and vitamin deficiencies however there isn’t yet enough evidence to support these as causative factors for the disease (18).
Genetics
As mentioned above, genetics are suspected to be a contributing factor to type 1 diabetes, however they don’t seem to be solely responsible. Many people hypothesize that certain genes create a higher risk of developing the disease which may occur when influenced by additional additive risk factors.
Many specialists think that people with diabetes have a genetic susceptibility to the disease that may only develop after an environmental trigger or exposure.
The triggers may be different for different people - and may involve a combination of multiple factors.
Type 1 Diabetes Treatment
The treatment initially may seem simple: Insulin. Insulin. Insulin. Right?
While this is the medicine used, insulin management can be delicate and become extremely complicated. While there needs to be enough insulin to control blood glucose, too much insulin leads to a blood sugar that can become dangerously low - called hypoglycemia.
While some people just use insulin injections, there are many different types of insulin and they may need to give themselves these injections in different combinations at different times throughout the day.
Other approaches include an ‘artificial pancreas’, which is a diabetic treatment approach that attempts to re-create a more automatic supply of insulin. An example of this is an insulin pump, which is a medical device that constantly monitors sugars and provides insulin as needed.
And while taking insulin consistently is critical to treatment, it’s not the only important element in managing the disease.
Maintaining as close to a normal blood glucose level as possible with minimal fluctuations and weight control are major goals of therapy (19).
This ideally involves eating a controlled and consistent amount of healthy carbohydrates throughout each day that is paired with the correct dosing of insulin. Each diabetic may process glucose differently and have unique insulin needs. It is therefore critical to work closely with a doctor and nutritionist when first diagnosed in order to determine and plan optimal nutritional intake and insulin administration.
Effective treatment of type 1 diabetes involves:
1) Minimizing Changes in Blood Glucose Levels
-
Regular exercise
-
Insulin Administration
2) Minimizing other Risk Factors for Diabetic Complications
-
Weight Control
-
Regular Exercise
1) Minimizing Changes in Blood Glucose Levels
A large part of minimizing fluctuations in blood glucose involves dietary modifications like managing carbohydrate intake, as well as accounting for physical activity and insulin administration.
Type 1 Diabetes Diet
It is critical for people with type 1 diabetes to carefully manage their diet and balance that with the appropriate insulin requirements.
Once eaten, carbohydrates turn into sugars and cause a spike in blood glucose. Diets too low or too high in carbohydrates can be challenging for type 1 diabetics as they can result in more fluctuations in glucose that make it more difficult to control. A somewhat lower intake in carbohydrates can contribute to improving overall blood sugar control.
Because everyone’s specific diet may differ based on their activity level and lifestyle, and each individual has a unique response to insulin, it’s very important to work with a doctor and nutritionist when initially determining your diet and getting used to your glucose management.
Basic Diabetic Diet Principles
- Learn What Makes a Good Carbohydrate
- Learn How to Count Carbohydrates
- Meal Plan
- Insulin Administration

LEAN PROTEIN
Including either meat or plant based lean protein in your diet provides significant health benefits. It gives your body the building blocks needed to repair tissue, build and maintain bones and muscle, and create many hormones and enzymes. Protein also helps weight loss by making you feel more satiated. In other words, it makes you feel more full and satisfied which leads many people to consume fewer calories and therefore lose weight.
UNSATURATED FATS
Yes, some fats are good for you! Monosaturated fats are considered ‘healthy fats’ because they can increase your 'good cholesterol' (HDL) and lower your 'bad cholesterol' (LDL). Some studies have also found them to help lower blood pressure when they are used to replace carbohydrates or unhealthy fats.
VEGETABLES
Leafy green vegetables get good press for a reason. They are packed with a variety of nutrients including vitamins, minerals and antioxidants that supports our bodily functions. Simultaneously they are very low in calories and high in fiber making them an even more ideal option for diabetics. Vegetables are considered a low digestible carbohydrate, making them a 'good carbohydrate' choice. All of these wonderful qualities make them ideal to eat in high volume. In other words, we can eat them in very large quantities for high nutritional value and very few calories.
FRUIT
Fresh fruit offers many health benefits. They are also high in fiber and contain many other nutrients including antioxidants and vitamins. They can be utilized as a way to avoid candy and other desserts. Eating fruit can satisfy our sweet tooth while providing rich nutritional value for very few calories. Because they still do contain some sugar, type 1 diabetics need to be careful about the amount of fruit they consume, and count it in with their carbohydrates for the day.
WHOLE GRAINS
Whole grains provide a slew of wonderful benefits for our health. They give us a superb source of fiber and are packed with a variety of other nutrients. Whole grains have been shown to reduce the risk of many chronic health conditions including heart disease, diabetes and some cancers. They have even been linked to a decrease in overall mortality. Like fruits, they also still need to be counted in the diabetics daily carbohydrate intake.
FIBER
Fiber not only helps with glycemic control, it’s shown to be good for us in many other ways including improving our intestinal health. Meeting the recommended 14 grams of fiber for every 1000 calories of food you consume can be easily accomplished by a diet filled with fruits, vegetables and whole grains. .
Diabetic Diets Should Avoid:
- Added Sugar
- Saturated Fats
- Processed Foods
- Salt
ADDED SUGAR
If you or a loved one is diagnosed with diabetes, eliminating added sugar should be one of the first things you tackle. This is easy to do by looking at labels where they clearly list ‘added sugar’. Added sugar is diabetes enemy - it has been shown to both be a cause of both the development and worsening of the disease. It leads to weight gain and causes high spikes in glucose while providing no nutritional value.
SATURATED FATS
Saturated fats should also be avoided. They cause a rise in ‘bad cholesterol’ (LDL) and therefore increase the risk of developing and/or progression of high cholesterol (hypercholesterolemia) and high triglycerides (hypertriglyceridemia as well as damaged blood vessels (atherosclerosis). All of this increases the risk of heart disease and other vascular diseases including stroke. Their high caloric content leads to weight gain without providing significant value.
PROCESSED FOODS
Processed foods tend to have a high glycemic index and be highly caloric dense without many nutrients.
SALT
A diet low in sodium (salt) (<2300mg/day) is recommended because it helps decrease other risk factors including high blood pressure. If you already have high blood pressure or heart disease, your doctor may recommend this number to be even lower.

Exercise for Diabetes
Incorporating regular exercise into your daily life is important for so many reasons. Not only does exercise independently improve glycemic control, weight loss and overall weight control, it also independently reduces the risk of other comorbid conditions including heart disease, high blood pressure and high cholesterol. It also is shown to overall improve mood and quality of life.
Benefits of Exercise:
- Improved Blood Sugar Control
- Weight Control
- Improved Emotional State
- Reduced Risk for Comorbid Diseases
2) Minimizing other Risk Factors for Diabetes Complications
It’s much more likely that you will suffer from serious complications of diabetes if you also have other risk factors for these conditions. In particular, obesity, hypertension and high cholesterol can all also contribute to these complications which include heart disease, stroke, infections, peripheral vascular disease, kidney disease and more.
Controlling Blood Pressure & Cholesterol
The good news about controlling hypertension and cholesterol is that their treatment and prevention involves the same principles as managing diabetes: diet modification, exercise and maintaining a healthy weight.
While diet and exercise are often enough to keep these conditions at bay, it requires consistently eating healthy and staying active to start seeing results if you’re already affected by these diseases. Therefore medications can be required to help control these conditions.
The goal is to be able to someday wean off of the medications once consistent diet and exercise take effect.
In rare case, medications may always be needed for adequate control.
Diabetes Weight Loss & Exercise
Many people with type 1 diabetes and even more individuals with type 2 diabetes are overweight. Obesity unfortunately contributes significantly to causing additional complications and increases overall morbidity and mortality.
Achieving a healthy weight and maintaining it is monumental for all of our health - and this is especially true for people with diabetes.
Determining the right calories to obtain your goal weight, and tracking them consistently is integral to successful weight loss. Exercise not only helps with weight loss but independently contributes to heart health and lowering other risk factors for diabetic complications.
Manage your diabetes the easy way with healthy, carb controlled meal plans delivered to your door each week!
